Periodontitis Dermatitis: Gum Disease's Skin Connection?
Periodontitis Dermatitis: Gum Disease's Skin Connection?
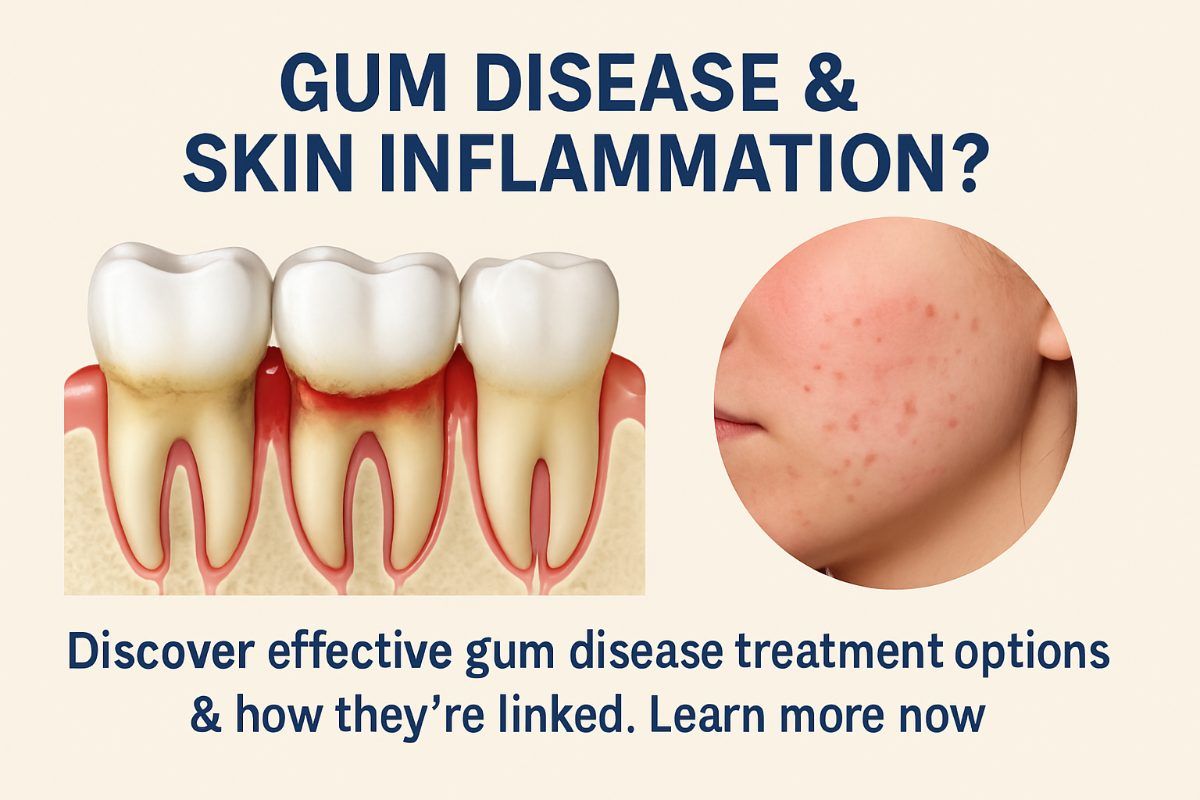
Periodontitis dermatitis describes skin inflammation that appears linked to severe gum infection. This short guide explains how chronic periodontal disease can show up as rashes or persistent skin lesions, why that connection matters, and what evidence-based gum disease treatment can reduce both oral and skin inflammation.
What Is Periodontitis Dermatitis?
Periodontitis dermatitis refers to skin changes—redness, rashes, pustules, or slow-healing patches—that occur alongside advanced periodontal disease. In these cases, inflamed gums and the bacteria that thrive there may trigger wider immune reactions or spread toxins that affect skin health. Recognizing the oral-skin link matters because treating the mouth can sometimes improve persistent dermatologic problems and reduce systemic inflammation that affects overall health.
How Gum Infection And Skin Inflammation Are Linked
Immune Response And Systemic Inflammation
Chronic gum infection keeps the immune system activated. That sustained immune signaling raises levels of inflammatory molecules in the blood, which can worsen skin conditions or make the skin slower to heal. Inflammation from the mouth is not strictly local—it can amplify immune reactions across the body.
Oral Bacteria And The Skin Microbiome
Pathogenic oral microbes release toxins and enzymes that can alter nearby tissues and, in some cases, influence the skin microbiome. Bacteria or their byproducts may travel through saliva, skin breaks, or the bloodstream and trigger localized skin inflammation or secondary infections in vulnerable areas.
Common Risk Factors
- Smoking or tobacco use
- Poor oral hygiene and untreated periodontal pockets
- Diabetes and other metabolic disorders
- Medications that affect immune response or oral flora
- Underlying immune or autoimmune conditions
Signs To Watch For: Gum And Skin Symptoms
Early recognition helps guide appropriate care.
- Periodontal signs: bleeding gums, swollen gums, deep periodontal pockets, gum recession, loose teeth, bad breath.
- Skin signs: persistent redness, recurring rashes or pustules near the mouth or lower face, slow-healing ulcers, or dermatitis that does not respond to typical topical care.
Tip: If skin problems regularly flare alongside gum symptoms or do not improve with dermatologic care alone, consider a combined dental and medical evaluation to look for a periodontal source.
Evidence-Based Gum Disease Treatment Options For Periodontitis Dermatitis
Non‑Surgical Periodontal Therapy
Initial therapy focuses on controlling infection and lowering inflammation. Scaling and root planing (deep cleaning) plus improved daily oral hygiene can dramatically reduce bacterial load. Many patients see notable improvement in skin inflammation once the oral infection is managed.
Minimally Invasive, Biologic Therapies
Laser-assisted therapies like LANAP promote pocket reduction and tissue healing while preserving healthy tissue. Platelet-rich fibrin (PRF) uses the patient’s own blood to speed soft tissue and bone healing. These tissue-preserving approaches reduce trauma and support faster resolution of inflammation.
Adjunctive Testing And Targeted Antimicrobials
Salivary and microbiome testing (for example, OralDNA®) can identify specific pathogens driving disease. Targeted antimicrobial treatments—such as localized ozone therapy or site-specific antimicrobials—allow precise control of harmful microbes. Systemic antibiotics are used selectively when testing and clinical signs indicate they are needed.
When Surgical Treatment Or Restorative Care Is Needed
Surgery may be indicated when deep bone loss, persistent pockets, or anatomical issues prevent healing with non-surgical care. Procedures can include flap surgery, bone grafting, or guided tissue regeneration. After infection control, restorative or implant therapy may be planned to restore function and prevent future disease.
Prevention And Home Strategies To Reduce Oral‑Skin Inflammation
- Brush twice daily with a soft brush and use interdental cleaning daily.
- Use antimicrobial mouth rinses only as recommended by your clinician.
- Follow an anti-inflammatory diet rich in whole foods, omega-3s, and antioxidants.
- Prioritize sleep, treat airway issues, and manage stress to support immune balance.
- Quit smoking and limit toxin exposures that aggravate immune responses.
How A Biologic, Multidisciplinary Practice Approaches Gum Disease Treatment
A biologic practice uses advanced diagnostics—salivary microbiome testing, CBCT imaging, and airway assessments—to find root causes of oral-systemic inflammation. At Tetrahealth, Drs. Alex and Michele Volchonok combine minimally invasive therapies like LANAP and PRF with targeted ozone and microbiome-informed care to treat both infection and the factors that sustain it. This collaborative model often includes dermatology and medical partners when skin symptoms persist, ensuring coordinated, toxin-free care that addresses oral and skin health together.
When To Seek Care And Next Steps
Seek evaluation if you notice bleeding gums, persistent bad breath, loose teeth, or skin lesions that won’t heal. Red flags include fever, rapidly spreading skin infection, or sudden tooth mobility. At a clinical assessment you can expect diagnostic testing, discussion of personalized gum disease treatment options, and a coordinated plan that may involve minimally invasive therapy, targeted antimicrobials, and medical collaboration. Schedule a clinical assessment with a periodontal specialist if oral and skin symptoms persist despite routine care.