Receding Gums - What Are They, And Can Implants Help?
Receding Gums - What Are They, And Can Implants Help?
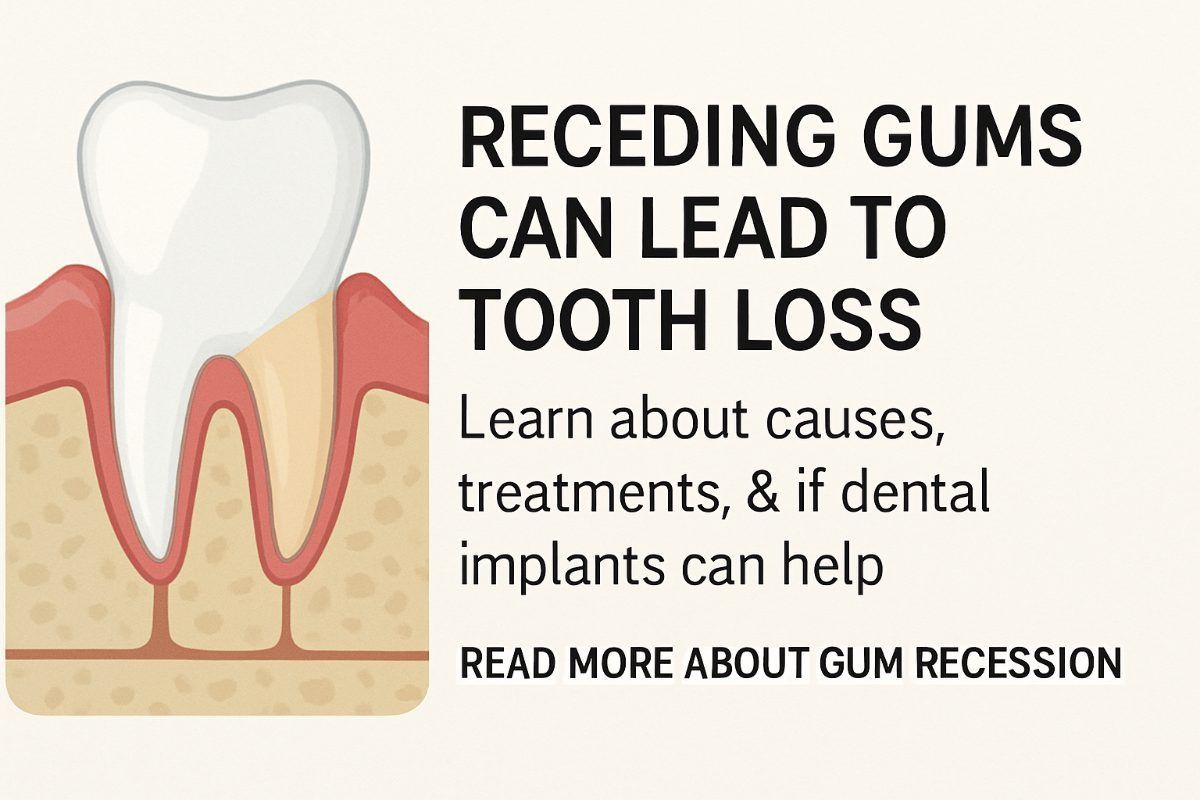
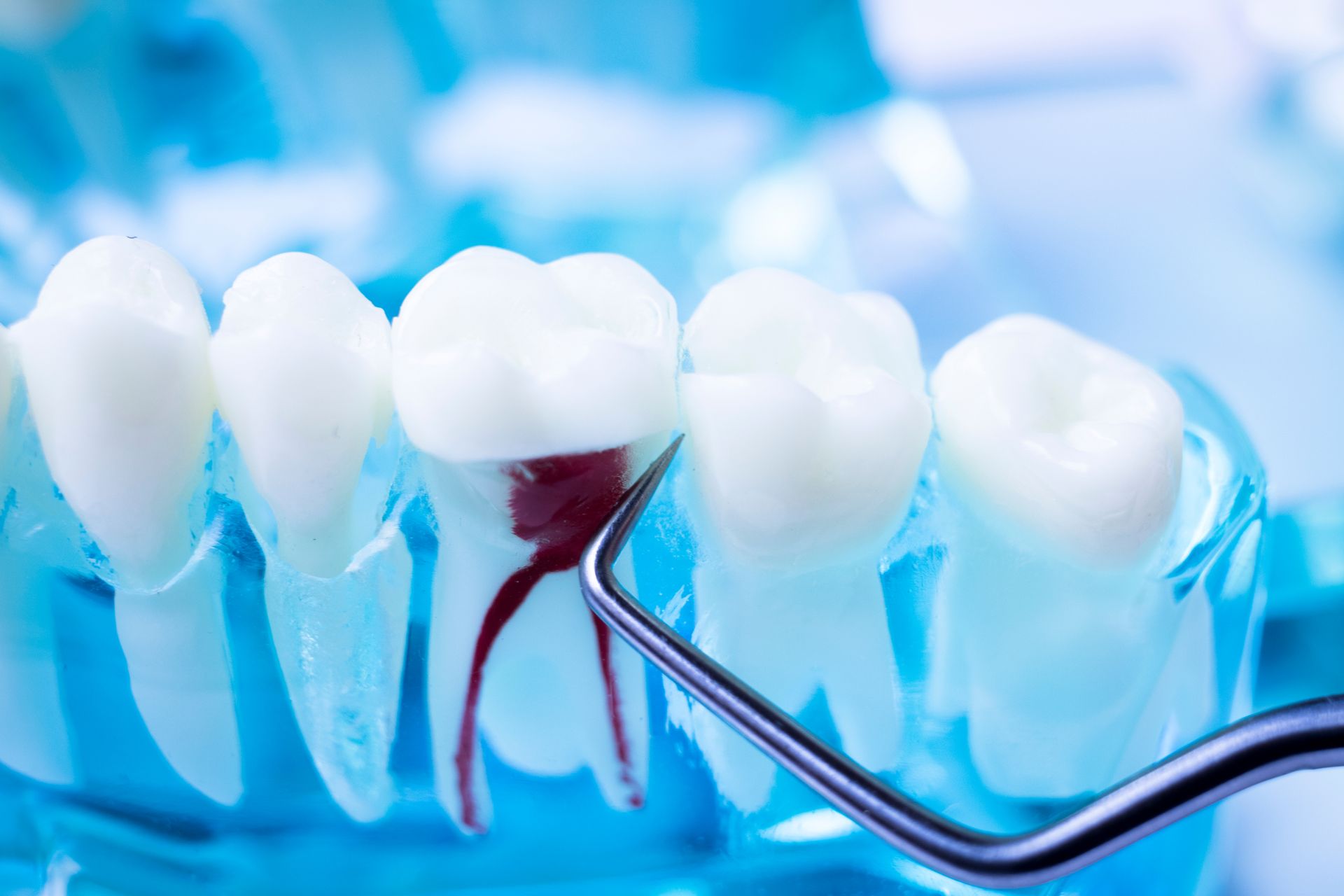
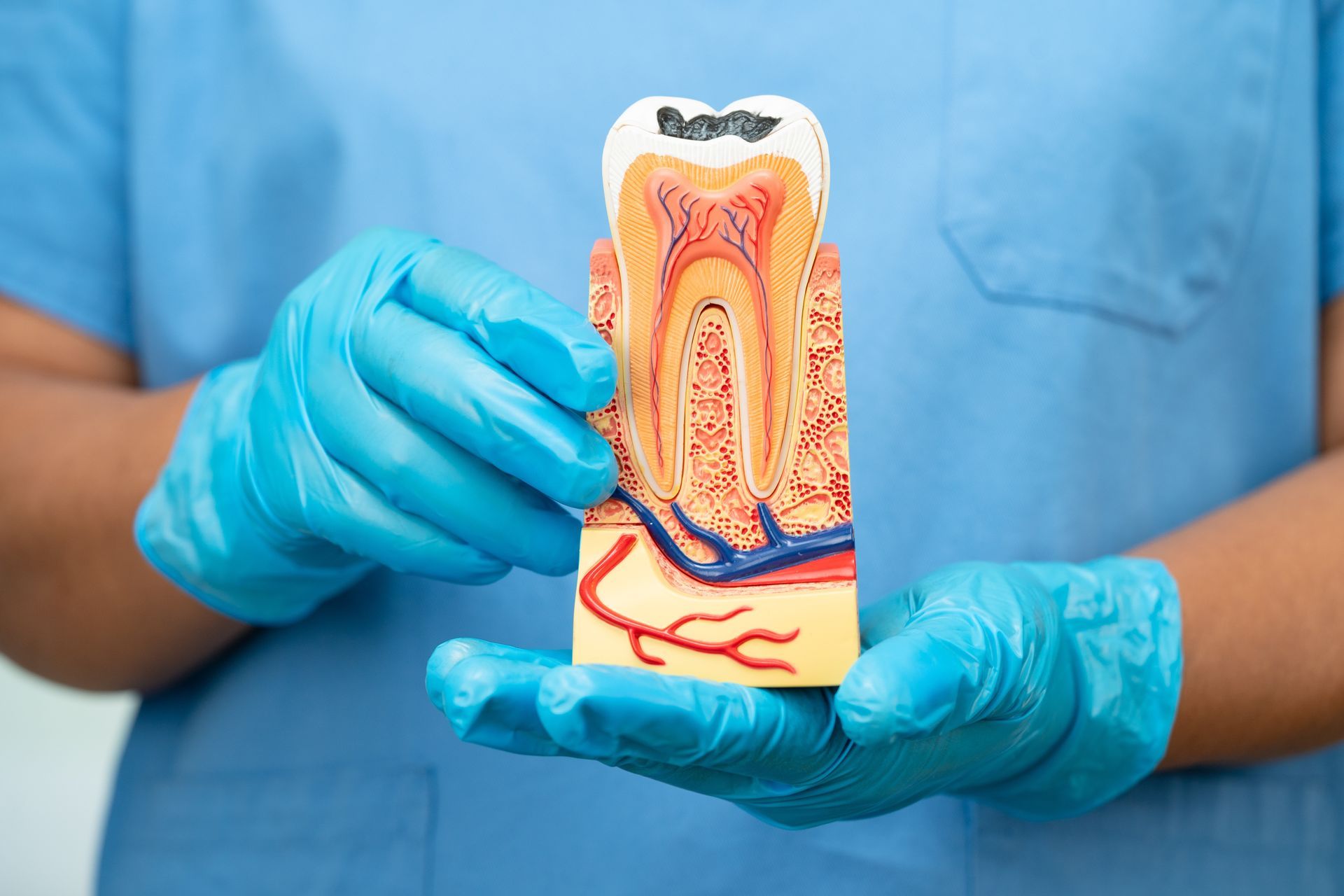
Receding gums occur when the gum tissue that surrounds teeth pulls back or wears away, exposing more of the tooth or its root. This condition matters because it can cause tooth sensitivity, make teeth look longer, create notches at the gumline, and eventually lead to tooth loss or infection if left untreated. Many patients ask: can dental implants help when gums have receded? This article explains what causes receding gums, how dentists diagnose the problem, treatment options to stop and repair recession, and when dental implants may be part of the solution.
What Are Receding Gums And What Causes Them?
Gum recession is the loss of gum tissue around a tooth so that the root becomes exposed. It is not the same as normal gum wear and can progress over time if the cause is not addressed. Receding gums can affect one tooth or many teeth and can change the way your smile looks.
Common Causes
- Gum disease (periodontitis) — infection that destroys tissue and bone
- Aggressive brushing or incorrect flossing technique
- Tobacco use and smoking
- Orthodontic tooth movement or tooth position that stresses gums
- Trauma, clenching, or grinding (bruxism)
- Genetics and systemic conditions such as diabetes or dry mouth
Common Signs Patients Notice
- Increased tooth sensitivity to hot, cold, or sweet
- Teeth that look longer than before
- Notches or grooves at the gumline
- Dark triangular spaces between teeth
- Loose teeth in advanced cases
How Dentists Diagnose The Severity Of Receding Gums
Diagnosis starts with a full clinical exam. A dentist or periodontist measures gum recession in millimeters using a periodontal probe and documents changes with photos or intraoral scans to track progression. Digital records make it easier to compare visits and spot worsening recession.
When more detail is needed, advanced imaging and tests are used:
- Cone Beam CT (CBCT) to evaluate bone level and plan grafting or implants
- ROSA™ screening to assess radiographic, oral, salivary, and airway health
- OralDNA® salivary testing to identify bacterial drivers and inflammation
Non-Surgical And Minimally Invasive Treatments To Stop Progression
Early-stage recession is often managed without surgery by removing the causes and supporting healing.
Behavior And Home Care
- Switch to a soft-bristled brush and use gentle technique
- Avoid aggressive flossing; use interdental brushes or water flossers as advised
- Quit tobacco and control grinding with a nightguard
- Address dry mouth and systemic health factors with your provider
Office Treatments
- Scaling and root planing to remove bacterial buildup
- Antimicrobial or ozone therapy to reduce infection
- Desensitizing agents to reduce sensitivity
- LANAP laser therapy and PRF to promote healing and reattachment
Surgical Options To Restore Lost Gum And Bone
Surgery is considered when recession is advancing, root exposure causes defects, or aesthetics are a major concern. Surgical techniques rebuild soft tissue and, when needed, underlying bone.
- Connective tissue grafts and free gingival grafts to replace missing gum
- Tunneling techniques that preserve blood supply and improve esthetics
- Guided tissue or bone regeneration to restore supporting bone
- Use of PRF or other biologic materials to speed healing and improve outcomes
Can Dental Implants Help Patients With Receding Gums?
Short answer: dental implants do not reverse recession of your natural gums. However, implants can replace teeth that have been lost because of severe periodontal disease or tooth failure related to advanced recession.
Typical pathway when implants are considered:
- Treat infection and control inflammation first (scaling, LANAP, antibiotics as needed, OralDNA testing)
- Regenerate bone and soft tissue when required with grafting, PRF, and guided regeneration
- Place the implant once the site is healthy; consider zirconia dental implants for a metal-free, biocompatible option
- Rebuild the soft tissue around the implant for a natural-looking gum line
Risks unique to implants include peri-implant mucositis and peri-implantitis — inflammatory conditions around implants that can cause bone loss. Careful planning with CBCT, ROSA diagnostics, biologic materials like PRF, and strict maintenance schedules reduces these risks. Dental implants can provide stable, long-term replacements when natural teeth cannot be saved.
Prevention, Long-Term Care, And When To See A Specialist
Preventing further recession and protecting your oral health requires consistent care and early attention to warning signs.
Practical Prevention Tips
- Brush gently with a soft brush and use proper technique
- Keep up with regular dental cleanings and exams
- Use a nightguard if you clench or grind
- Stop smoking and manage systemic health issues like diabetes
- Address airway or sleep issues that can worsen grinding and inflammation
Red Flags To See A Periodontist Or Implantologist
- Rapid or noticeable gum recession
- Persistent bleeding, pain, or exposed roots
- Loose teeth or failing prior treatments
- Ongoing infection despite home care
Tetrahealth offers biologic, minimally invasive options to treat the root causes of gum recession and plan restorative care. Drs. Alex and Michele Volchonok are board‑certified specialists who use advanced diagnostics (CBCT, ROSA, OralDNA), LANAP, PRF, and zirconia implants to prioritize healing and long-term health. Their offices are in Manhattan, NY and Greenwich, CT.
What To Bring To Your Consult
When you schedule a consult for receding gums or to discuss dental implants, bring:
- A list of symptoms and when you first noticed them
- Recent dental records, X-rays, or intraoral scans if you have them
- Your dental history, prior treatments, and any failed restorations
- Current medications and health conditions
A specialist will review history, perform a clinical exam, take imaging or saliva testing as needed, and propose a personalized plan that may include non-surgical care, grafting, or dental implants when appropriate. Early evaluation gives you the best chance to stop progression and preserve both gum and tooth health.